Geographic Tongue
| Geographic Tongue | |
|---|---|
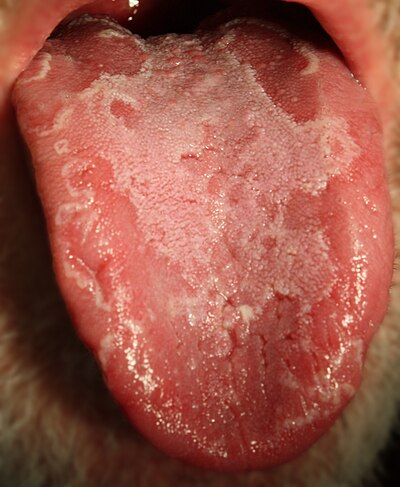 | |
| Characteristic map-like appearance of geographic tongue |
- A common condition of the mucous membrane of the tongue characterised by areas of smooth, red depapillation
- Areas can migrate over time
- The name comes from the map-like appearance of the tongue (patches resemble islands of an archipelago)
- Also known as:
- Benign migratory glossitis
- Erythema migrans
- Erythema migrans lingualis
- Glossitis areata exfoliativa
- Glossitis areata migrans
- Lingua geographica
- Psoriasiform mucositis
- Stomatitis areata migrans
- Wandering rash of the tongue
- Transitory benign plaques of the tongue
Epidemiology[edit | edit source]
Clinical Features[edit | edit source]
- Usually affects the dorsum of the tongue but on occasion can affect the ventrum
- Irregular, pink or red depapillated/atrophic areas
- Red areas are often well-demarcated and surrounded by distinct white/yellowish and slightly raised margins
- There is increased thickness of the intervening filiform papillae.
- Lesions can change in shape, size and location
- A lesion may start as a white patch before depapillation occurs
- Fissured tongue can occur with geographic tongue
- Usually asymptomatic but in a minority can cause sore mouth (pain/burning)
- Can be worsened by acidic foods (tomatoes/citrus), spice or cheese
- People with symptoms often report worsening at periods of emotional stress
Differential Diagnosis[edit | edit source]
Oral candidiasis
Oral Lichen Planus
Trauma
Oral psoriasis (rare)
Herpes simplex
Systemic lupus erythematosus
Oral leukoplakia
Aetiology and Pathogenesis[edit | edit source]
Aetiology[edit | edit source]
- Largely unknown but some associations[3]
- 4% of cases are associated with psoriasis (especially pustular psoriasis)[1]
- It is also seen in patients with a food allergy, allergic contact dermatitis, asthma, atopic dermatitis, reactive arthritis, anaemia, hormonal disturbance, emotional stress and in patients with early-stage of type 1 diabetes[3]
- An inverse relationship to smoking and tobacco use has been reported [4]
- Can run in families - raising suggestion of genetic predisposition[3]
- Reports of links with various human leukocyte antigens (increased incidence of HLA-DR5, HLA-DRW6 and HLA-Cw6 and decreased incidence in HLA-B51)[5]
- A hormonal relationship has also been reported[6]
Investigations[edit | edit source]
- Diagnosis is usually based on history and clinical examination
- Blood tests may be helpful to rule out differentials
- Biopsy and histologic examination of the lesions may also assist in excluding differentials and in reassuring patients of the benign nature of the disorder
Laboratory Investigations[edit | edit source]
- Routine laboratory tests, including full blood count, sedimentation rate, and levels of C-reactive protein and glucose, are usually normal
- Vitamin B12, ferritin and folate are usually normal
Histology[edit | edit source]
- Histopathological findings are very similar to those seen in psoriasis
- Characteristic features:
- Regular increase of the spinous layer with thickening of the lower portions
- Thickening and swelling of papillae
- Suprapapillary hypotrophy with occasional presence of a small spongiform pustule
- Absence of granular layer
- Parakeratosis
- Presence of Munro's microabscess
- Inflammatory cell infiltration in submucosa (particularly T-lymphocytes, macrophages and neutrophils)

Management[edit | edit source]
- Reassurance regarding the benign nature of the condition is usually all that is needed
- Symptomatic cases:
- Can be advised to avoid irritants in diet
- Maintain good oral hygiene
- Topical zinc may be helpful (Zinc sulphate 125mg dispersible tablet [Solvazinc] dissolved in water and used as a mouth rinse - three times a day for 3 months)
- Benzydamine hydrochloride 1.5mg/mL (0.15%) as mouthwash or spray (sugar-free) can also be used four times daily as instructed (15mL as rinse or four sprays every 1.5 hours as required)
Prognosis and Complications[edit | edit source]
- No long term sequelae
- May disappear over time but no method exists to predict cases that will
Follow-up[edit | edit source]
- Appropriate for monitoring and management in primary care
References[edit | edit source]
- ↑ 1.0 1.1 Scully C, Felix DH. Oral Medicine—Update for the dental practitioner Red and pigmented lesions. British dental journal. 2005 Nov;199(10):639-45.
- ↑ Jainkittivong A, Langlais RP. Geographic tongue: clinical characteristics of 188 cases. J contemp dent pract. 2005 Feb 15;6(1):123-35.
- ↑ 3.0 3.1 3.2 Assimakopoulos D, Patrikakos G, Fotika C, Elisaf M. Benign migratory glossitis or geographic tongue: an enigmatic oral lesion. The American journal of medicine. 2002 Dec 15;113(9):751-5.
- ↑ Shulman JD, Carpenter WM. Prevalence and risk factors associated with geographic tongue among US adults. Oral diseases. 2006 Jul;12(4):381-6.
- ↑ Picciani BL, Domingos TA, Teixeira-Souza T, Santos VD, Gonzaga HF, Cardoso-Oliveira J, Gripp AC, Dias EP, Carneiro S. Geographic tongue and psoriasis: clinical, histopathological, immunohistochemical and genetic correlation-a literature review. Anais brasileiros de dermatologia. 2016 Jul;91:410-21.
- ↑ Waltimo J. Geographic tongue during a year of oral contraceptive cycles. British dental journal. 1991 Aug;171(3):94-6.